New Research Reveals Financial Sacrifices Made by People who Provide Alzheimer’s Care
Results from a nationwide survey of 3500 Americans revealed that very few people are prepared for the cost of caring for someone with Alzheimer’s disease. The personal financial support required by a person with Alzheimer’s may ultimately deprive care contributors of basic necessities, such as food, transportation and medical care, according to the survey report, titled 2016 Alzheimer’s Disease Facts and Figures.
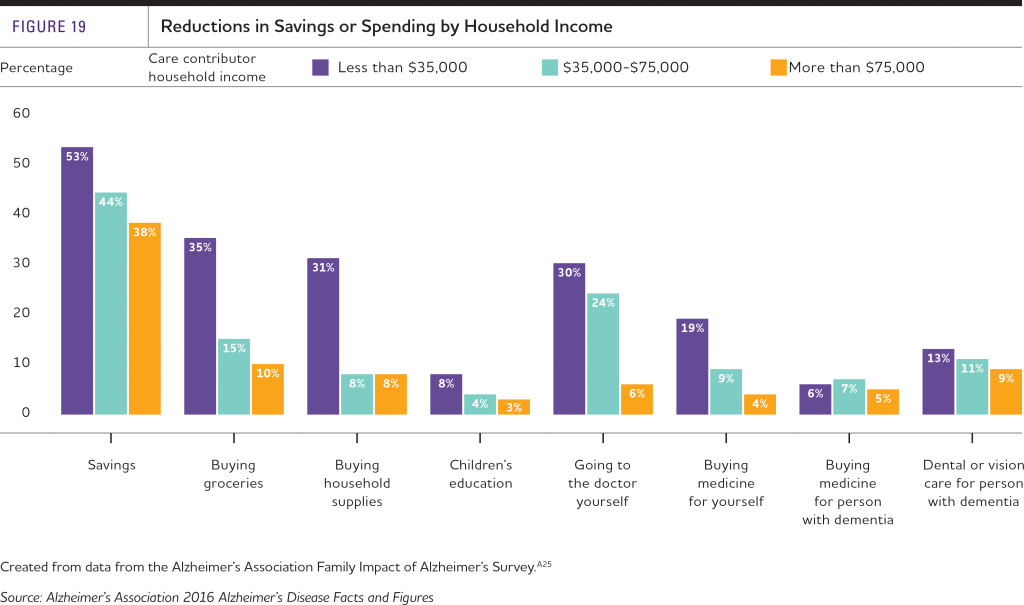 The data show that care contributors reduced their expenditures on basic necessities such as groceries or medicine (see chart). Overall, care contributors were 28 percent more likely to eat less or go hungry while contributing care to someone with Alzheimer’s, and one-fifth of them sacrificed their own medical care by cutting back on doctor visits. Overall, nearly half of care contributors cut back on their own expenses to afford dementia-related care for their family member or friend.
The data show that care contributors reduced their expenditures on basic necessities such as groceries or medicine (see chart). Overall, care contributors were 28 percent more likely to eat less or go hungry while contributing care to someone with Alzheimer’s, and one-fifth of them sacrificed their own medical care by cutting back on doctor visits. Overall, nearly half of care contributors cut back on their own expenses to afford dementia-related care for their family member or friend.
“Our social workers provide care consultations and support for families every single day, and they see it all,” said Elizabeth Edgerly, Ph.D., Chief Programs Officer with the Alzheimer’s Association, Northern California and Northern Nevada. “People are choosing between care for their mother and college for their daughter; or between quitting their job and figuring out how to pay for a caregiver. The choices are rarely easy ones.”
Today it is estimated that 5.4 million Americans have Alzheimer’s disease, and nearly 16 million family members and friends are caregivers providing financial, physical and emotional support. Financial depletion related to the support of someone living with Alzheimer’s can occur directly when family and friends contribute to in-home care or other health care resources.
The Alzheimer’s Association Facts and Figures report found that 13 percent of care contributors sold personal belongings, such as a car, to help pay for costs related to dementia, while nearly half tapped into savings or retirement funds. On average, care contributors, many of whom do not live with the person they’re caring for, spent more than $5,000 a year of their own money to care for someone with Alzheimer’s disease; however, amounts varied with many spending tens of thousands of dollars per year.
The financial burden of dementia is compounded for many care contributors, as more than one-third reported having to reduce their hours at work or quit their job entirely while caring for someone with Alzheimer’s, leading to an average loss of income of around $15,000 compared to the previous year. Eleven percent of care contributors have cut back on spending for their children’s education in order to provide support.
Preparing for the Financial Impact of Alzheimer’s
Unfortunately, a significant number of care contributors today don’t have a complete understanding of the financial implications of supporting someone with Alzheimer’s. According to data from the Alzheimer’s Association Facts and Figures report, about two out of three people incorrectly believe that Medicare will help them cover nursing home costs, or they are not sure whether the costs will be covered. At the current time, only three percent of adults in the U.S. carry long-term care insurance that might help them cover these costs.
“Part of the work we do with families is to help them prepare and proactively plan for the potential financial impact of Alzheimer’s disease,” said William H. Fisher, Chief Executive Officer of the Alzheimer’s Association, Northern California and Northern Nevada. “People might have a retirement plan in place, but that plan usually assumes that Medicare will cover the medical care they need.”
To help care contributors financially plan for the future, the Alzheimer’s Association suggests the following:
- Look at retirement planning as a time to think about how to prepare for the need for long-term medical care. After an Alzheimer’s diagnosis, your options may be more limited.
- Conduct an inventory of your financial resources (for example, savings, insurance, retirement benefits, government assistance, VA benefits, etc.). A financial planner or elder care attorney can help with this.
- Investigate long-term care services (for example, home care, assisted living residences and nursing homes) in your area. Ask what types of insurance they accept and if they accept Medicaid as few individuals with Alzheimer’s and other dementias have sufficient long-term care insurance or can afford to pay out-of-pocket for long-term care services for as long as they are needed.
- Call the local Agency on Aging to determine what community services and support programs are available (for example, respite care, homemaker services and Meals on Wheels can help alleviate financial burdens).
- Once you understand what you have for financial resources and what you can afford, make a plan with your family or a close friend for how to access care.
To increase assistance for families affected by Alzheimer’s, the Alzheimer’s Association also supports the HOPE for Alzheimer’s Act, which would provide Medicare coverage for comprehensive care planning services following an Alzheimer’s or dementia diagnosis. Individuals can ask their legislator to co-sponsor and support the HOPE for Alzheimer’s Act.
Alzheimer’s Disease By The Numbers
The 2016 Facts and Figures report provides an in-depth look at the prevalence, incidence, mortality and economic impact of Alzheimer’s disease and other dementias – all of which continue to rise at staggering rates as the American population ages.
Prevalence, Incidence and Mortality
- An estimated 5.4 million Americans have Alzheimer’s disease in 2016. This includes an estimated 5.2 million people age 65 and older, and approximately 200,000 individuals under age 65 who have younger-onset Alzheimer’s. Barring the development of medical breakthroughs, the number will rise to 13.8 million by 2050.
- In California, 610,000 people over 65 have Alzheimer’s disease in 2016.
- Every 66 seconds, someone in the U.S. develops Alzheimer’s. By mid-century, someone in the U.S. will develop the disease every 33 seconds.
- Approximately 476,000 people””almost half a million””age 65 or older will develop Alzheimer’s in the U.S. in 2016.
- Two-thirds (3.3 million) of Americans over age 65 with Alzheimer’s are women.
- Alzheimer’s disease is the sixth-leading cause of death in the U.S., and the fifth-leading cause of death for those age 65 and older. In California, 11,891 people died with Alzheimer’s in 2013. From 2000-2013, the number of Alzheimer’s deaths increased 169% percent, while deaths from other major diseases, such as heart disease, breast cancer and HIV, decreased.
Cost of Paid and Unpaid Care
- Alzheimer’s is the costliest disease to society. Total national cost of caring for those with Alzheimer’s and other dementias is estimated at $236 billion (excludes unpaid caregiving), of which $160 billion is the cost to Medicare and Medicaid alone.
- In 2015, the nearly 16 million family and other unpaid caregivers of people with Alzheimer’s disease and other dementias provided an estimated 18.1 billion hours of unpaid care, a contribution to the nation valued at $221.3 billion (with care valued at $12.25 per hour).
- In 2015 there were 1,592,000 Alzheimer’s caregivers in California providing 1.8 billion hours of unpaid care valued at $22.2 billion.
- Total payments for health care, long-term care and hospice for people with Alzheimer’s and other dementias are projected to increase to more than $1 trillion in 2050 (in current dollars) from $236 billion in 2016.
- The financial toll of Alzheimer’s on individuals exceeds the toll on Medicaid. Total Medicaid spending for people with Alzheimer’s disease is $43 billion, while out-of-pocket spending is estimated at $46 billion, or 19 percent, of total care payments for those with Alzheimer’s and other dementias.
“The statistics are overwhelming, we know,” said Mr. Fisher. But the Alzheimer’s Association of Northern California and Northern Nevada is here to support families throughout their journey, and to advocate for policy changes that will improve the current state of affairs.”
Full text of the Alzheimer’s Association 2016 Alzheimer’s Disease Facts and Figures report can be viewed at alz.org/facts.
Helpful information related to this post:


















I was not sure if my first attempted blog got through. it was as follow
I wonder how these financial figures would change if they included the total number of people affected with the entire family of dementia’s like lewy bodies, frontal lobe, vascular and etc.?
I would guess it would be even more alarming.