Can a newly approved test diagnose Alzheimer’s?
 Scientists are not absolutely sure what causes brain cell death and tissue loss in Alzheimer’s disease, but two abnormal brain lesions – known as amyloid plaques and tau tangles – are prime suspects. Amyloid plaques are abnormal clusters of protein fragments that build up between nerve cells in the brain that form when fragments of the amyloid protein clump together.
Scientists are not absolutely sure what causes brain cell death and tissue loss in Alzheimer’s disease, but two abnormal brain lesions – known as amyloid plaques and tau tangles – are prime suspects. Amyloid plaques are abnormal clusters of protein fragments that build up between nerve cells in the brain that form when fragments of the amyloid protein clump together.
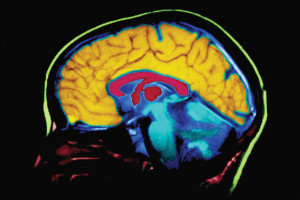
The U.S. Food and Drug Administration (FDA) recently approved florbetapir (Amyvid), a radioactive dye for use with PET scans for detecting the buildup of amyloid plaque in the brain. With this approval came many news stories claiming this would be a new test to detect Alzheimer’s, but it’s not exactly that simple.
The Claim
According to the prescribing information, Amyvid is “for PET imaging of the brain to estimate beta-amyloid neuritic plaque density in adult patients with cognitive impairment who are being evaluated for Alzheimer’s disease and other causes of cognitive decline.” Basically, if a PET scan using Amyvid shows an absence or a low density of amyloid plaques, the individual’s dementia is likely caused by something other than Alzheimer’s disease. If the scan does find amyloid plaque buildup, there is an increased likelihood that the individual’s memory impairment is caused by Alzheimer’s.
Beyond the Headline
Several points of clarification need to be made in regards to the use of Amyvid.
Amyloid plaque buildup does not necessarily mean Alzheimer’s: This test indicates how much amyloid plaque is present in the brain. While plaques are certainly present in individuals with Alzheimer’s, they may also be present in individuals with other types of neurological conditions as well as older people with normal cognition. Presence of amyloid plaque increases the likelihood of having Alzheimer’s disease, but that is NOT a diagnosis. A good analogy is high cholesterol as an indicator of heart attack. Not everyone who has high cholesterol has a heart attack; on the other hand, people that don’t have high cholesterol can still have a heart attack.
Who should take this test: There is currently not enough research to know what a positive amyloid scan means in people without significant memory impairment. This is why the vast majority of researchers recommend against people with normal cognition getting an amyloid scan. For people who have memory problems or mild cognitive impairment (MCI), this test may indicate an increased likelihood of developing Alzheimer’s disease dementia over the next few years, but this research is ongoing. If after a thorough evaluation there remain questions about the diagnosis or the type of dementia, then this test may be appropriate and may help to support or refute the diagnosis of Alzheimer’s.
Cost and coverage: In general, PET scans can cost between $1,000 and $3,000. Insurers often lag behind the FDA approval, so it is unlikely that insurance will cover the test immediately and it’s not clear when or if this test will be covered by insurance. If it is eventually covered, insurers may put conditions on payment. For example, people may need to have a full clinical examination before getting this scan.
The bottom line
The approval of florbetapir is very exciting and we hope that by being widely available in the field, it will lead to the pursuit of better Alzheimer’s diagnostics, treatments and preventions. However, the exact use of florbetapir-PET imaging remains unclear. There is a real possibility that this tool will be offered to individuals with less than realistic promises about its value. As such, we recommend that people get access to this test only in the context of a complete evaluation of medical/neurological status and with appropriate expert consultation.
Stay tuned for more information on this topic as the Alzheimer’s Association has convened a task force with the Society of Nuclear Medicine to develop recommendations for the use of amyloid imaging for physicians, imaging and other medical specialists, Alzheimer’s families and the general public. It is planned that the recommendations will be unveiled later this year.
Helpful information related to this story
Know the 10 Signs of Alzheimer’s
What is dementia and what causes it?
For more information on the latest news and developments in Alzheimer’s research, visit www.alz.org/research.


















Thanks for the writeup! very informative. I was not aware of the realease of Amyvid
I wonder if the new test to detect Alzheimer’s Disease will help get more information leading to treatment or even a cure!
Great article and let’s all hope!
Interestingly, I found this from about a year ago this month about diagnosing guidelines form the NIH as well.
http://www.nih.gov/news/health/apr2011/nia-19.htm